Diabetes damages small blood vessels in the retina. Patients with diabetes may have:
- normal, healthy retina
- microscopic abnormalities that are visible on examination and signs of early disease, but which do not do not require treatment
- abnormalities in the retina that may or may not impact vision currrently but require treatment in the office to prevent risk of severe vision loss
- abnormalities in the retina with vision decrease or loss that require surgery
The only way to distinguish between the above entities is to undergo a careful, dilated retinal examination by an experienced eye doctor. Timely, effective diagnosis and treatment of diabetic retinopathy is highly effective at maintaining vision and preventing vision loss.
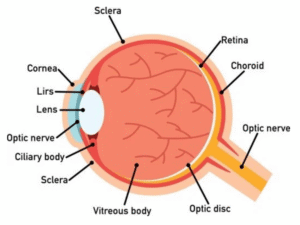
What is the Retina?
- If the eye were a camera, the retina would be the film of that camera
- The retina is a thin sheet of nerve cells that lines the inside back wall of the eye
- Light travels through the eye and ultimately reaches photoreceptors, the light-sensitive cells in the retina
- The signal from the photoreceptors then travel along the optic nerve to the brain, where the signals are interpreted as vision
How Does Diabetes Effect the Retina?
- Diabetes causes damage to microscopic blood vessels in the retina
What Are the Different Types of Diabetic Retinal Disease (Diabetic Retinopathy)?
- The 2 main categories of diabetic retinopathy are nonproliferative diabetic retinopathy (NPDR) and proliferative diabetic retinopathy (PDR)
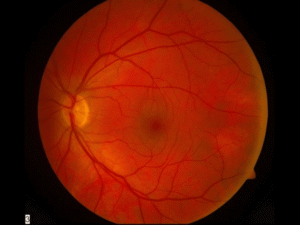
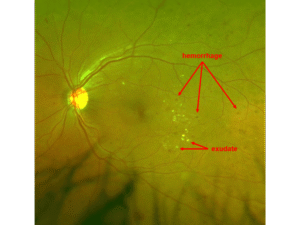
- Nonproliferative diabetic retinopathy (NPDR)
- There is damage to microscopic blood vessels, leading to bleeding, aneurysms, loss of blood flow, and/or swelling
- Vision may be excellent or severely decreased
Proliferative Diabetic Retinopathy (PDR)
- Diabetic damage to retinal blood vessels creates areas of loss of blood flow in the retina.
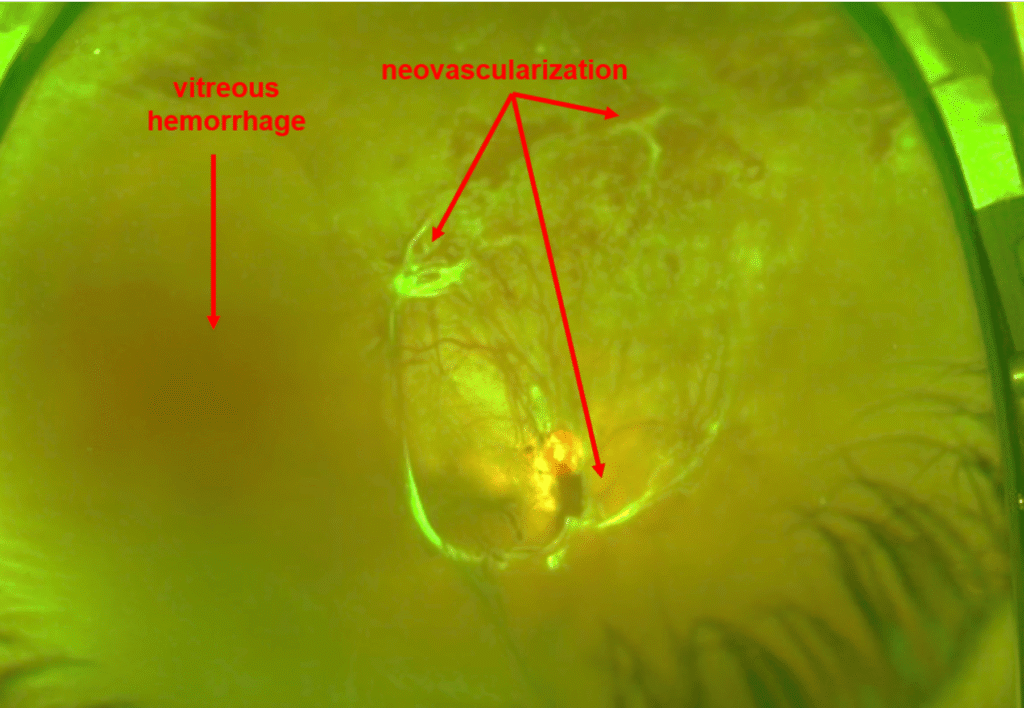
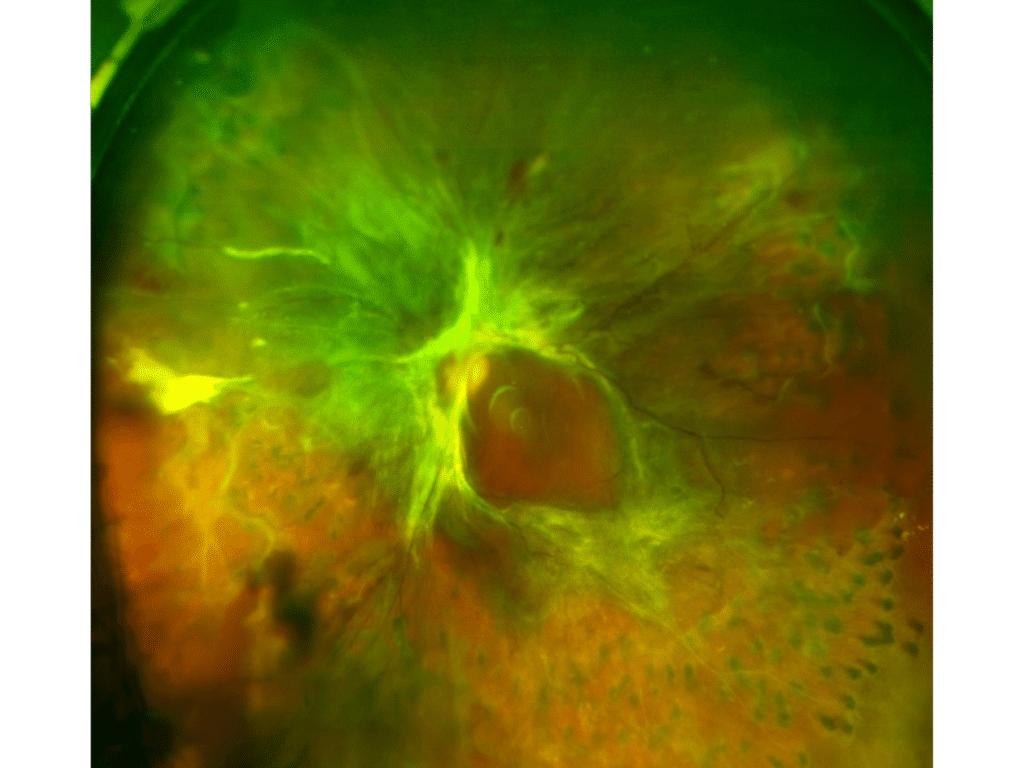
- The retina responds to loss of blood flow by making “new” blood vessels (called “neovascularization”)
- Unfortunately, the new blood vessels do not replace lost blood flow. Rather, they grow on the surface of the retina and cause vision loss in one of two ways:
- Vitreous hemorrhage
- Bleeding into the eye
- Instead of being filled with clear fluid through which one can see, the back of the eye is filled with blood, causing vision loss
- Tractional retinal detachment
- The new blood vessels pull on the retina (create “traction”) and pull the retina off the eye wall (“retinal detachment”)
- The photoreceptors in detached retina cannot see and undergo damage, resulting in severe vision loss, sometimes irreversible vision loss
- Vitreous hemorrhage
Diabetic Macular Edema (DME)
-
- Patients with either NPDR or PDR may develop diabetic macular edema
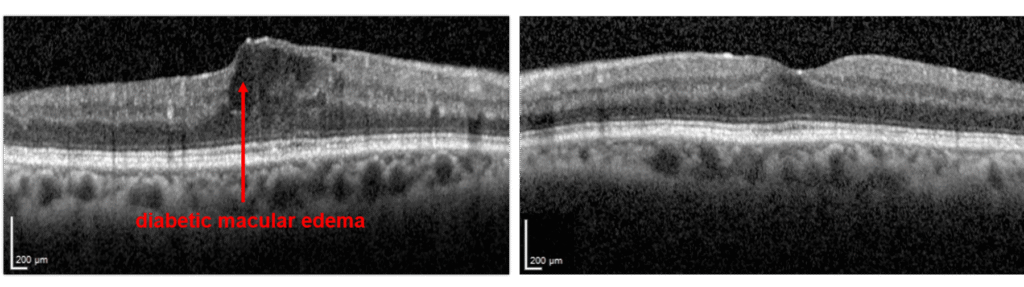
- Edema means “swelling”
- Blood vessels damaged by diabetes are leaky, and the fluid that leaks from these vessels accumulate in the retina
- The macula is the centermost part of the retina, which is responsible for much of high quality vision
- When diabetes causes swelling in the macula, one has “diabetic macular edema”
What Kind of Tests Will Be Performed to Evaluate for Diabetic Retinopathy?
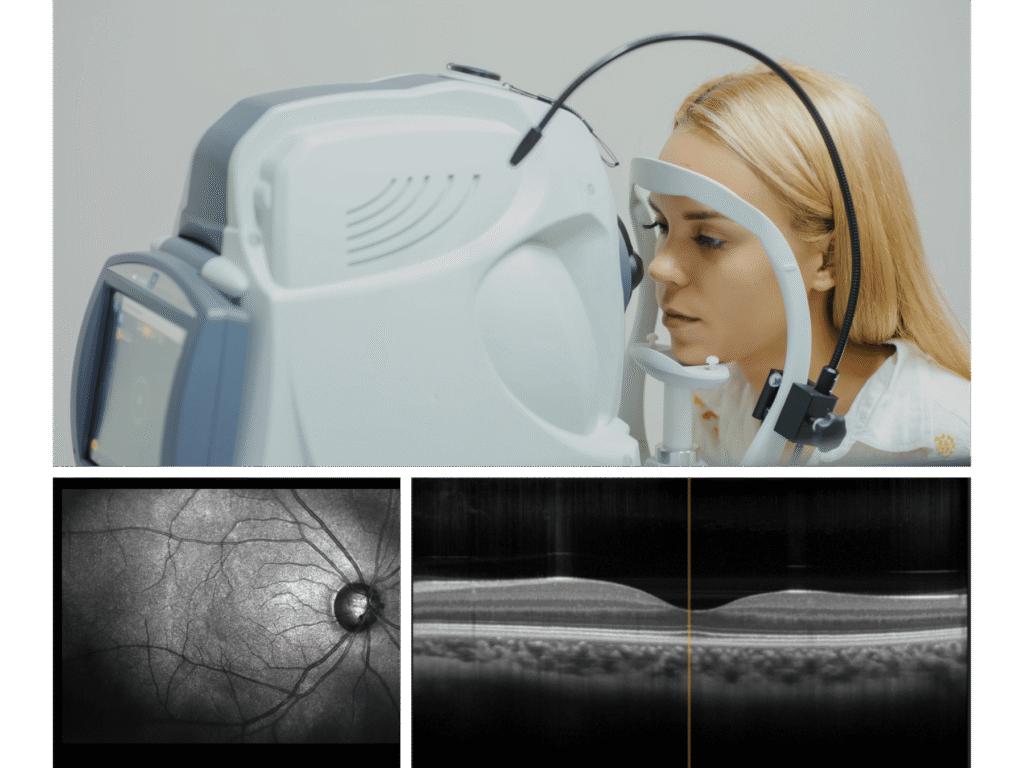
- Dilated retinal examination
- Optical coherence tomography (a scan to look for swelling in the retina (DME))
In some patients:
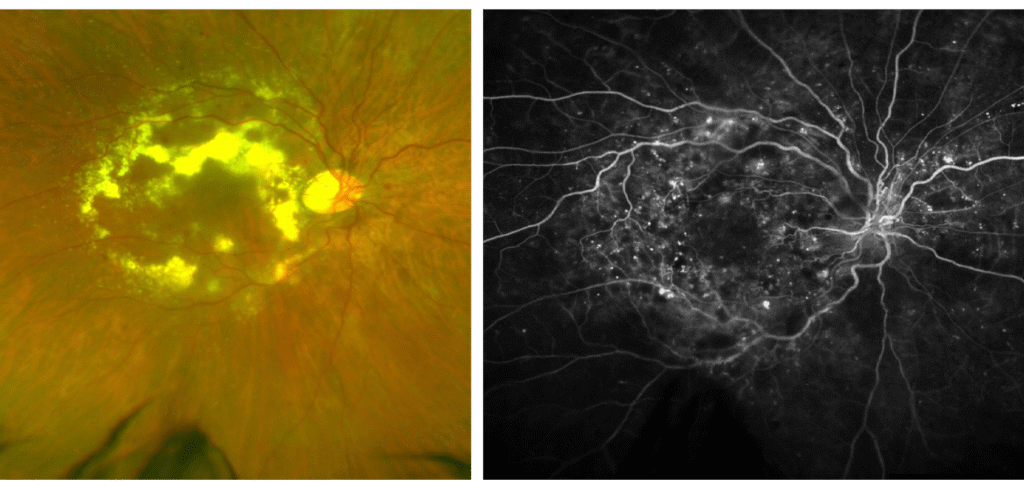
- Fluorescein angiography
- A dye is injected into the arm, from which to travels through the blood to the eye.
- Photographs are taken of the eye which map out all the blood vessels and blood flow in the retina
- This test identifies areas of blood flow loss as well as areas of new blood vessel grown (neovascularization)
- B-scan ultrasound
- Painless procedure whereby an ultrasound is performed over the closed eyelid to evaluate the retinal anatomy in eyes where hemorrhage prevents visualization of retinal details through the eye exam alone
How is Diabetic Macular Edema (DME) Treated?
- Blood sugar and blood pressure control significantly reduces the risk of diabetic retinopathy and its progression
- Intravitreal injections
- These medications are injected into the eye after drops are given to numb the eye
- Injections are given in the office. The drops are given over 5-10 minutes to clean and numb the eye, and the injection itself takes only seconds
- There are 2 types of medications that can be used
- Anti-vascular endothelial growth factor (anti-VEGF) injections
- Names: Avastin (bevacizumab), Lucentis (ranibizumab), Eylea (aflibercept), Vabysmo (faricimab), and others.
- A substance called VEGF causes the retinal blood vessels to be leaky to cause DME. These drugs block VEGF. Vabysmo works by blocking not only VEGF, but also Ang2, another molecule that is involved in diabetic retinopathy.
- Steroids
- Names: Triessence (triamcinolone), Ozurdex implant (dexamethasone, lasts several months), Iluvien implant (fluocinolone, lasts several years)
- Inflammation contributes to diabetic retinal disease and DME. Steroids reduce inflammation.
- Anti-vascular endothelial growth factor (anti-VEGF) injections
- Observation
- Mild cases of DME with excellent vision may be monitored without treatment
- Occasionally, laser (in the office) or surgery may also be recommended for DME
How is Nonproliferative Diabetic Retinopathy Treated?
- Blood sugar and blood pressure control significantly reduces the risk of diabetic retinopathy and its progression
- If there is diabetic macular edema, it is treated as above.
- In the absence of diabetic macular edema, management options for nonproliferative diabetic retinopathy include:
- Observation
- Treatment with anti-VEGF agents described above (Avastin, Lucentis, Eylea, Vabysmo, and others)
- Studies suggest that treatment with anti-VEGF agents reverses diabetic retinopathy and reduces progression of retinopathy. However, this must be balanced against the treatment burden and risks of treatment in eyes without macular edema.
How is Proliferative Diabetic Retinopathy Treated?
- Blood sugar and blood pressure control significantly reduces the risk of diabetic retinopathy and its progression.
- Laser (in the office)
- Intravitreal injections with anti-VEGF drugs described above (avastin, Lucentis, Eylea, Vabysmo, and other)
- A combination of injections and laser
- If there is vitreous hemorrhage or tractional retinal detachment, surgery may be necessary (see below)
How is Vitreous Hemorrhage From Proliferative Diabetic Retinopathy Treated?
- Blood sugar and blood pressure control significantly reduces the risk of diabetic retinopathy and its progression
- Observation / medical management
- Vitreous hemorrhage may resolve on its own
- Observation is therefore an option, especially in eyes without dense hemorrhage or very severe PDR
- Injections of anti-VEGF drugs may be given, and after the hemorrhage resolves, laser may be performed (laser cannot be performed through hemorrhage)
- If the hemorrhage fails to clear or other complications are noted, surgery may be indicated
- Surgery
- Pars plana vitrectomy surgery
- The hemorrhage is removed, the traction from the new blood vessel (neovascularization) membranes is relieved, and laser is applied to allow the neovascularization to regress
- An injection of anti-VEGF medication may be given prior to surgery to reduce intraoperative and postoperative complications risk
Request Appointment
Areas of Expertise
Patient Reviews
Posted onTrustindex verifies that the original source of the review is Google. Cannot say enough about the level of expertise and competency of Dr Hwang and his staff. He saved my vision by repairing a detached retina in my right eye and has been providing incredible care in treating my macular condition and retaining my vision over the years. He is caring and compassionate with a true love for his practice. I am blessed to be one of his patients!Posted onTrustindex verifies that the original source of the review is Google. Check up on visual issue went perfectly. Great staff as well.Posted onTrustindex verifies that the original source of the review is Google. Professional and thoughtful doctor, caring patient as a family member.Posted onTrustindex verifies that the original source of the review is Google. Great service. Very satisfied.Posted onTrustindex verifies that the original source of the review is Google. I have tremendous anxiety prior to my intraocular injections to manage my wet AMD, but Dr. Hwang makes the process as quick and painless as possible. I wouldn't trust my eye health to anyone else. He's the best.Posted onTrustindex verifies that the original source of the review is Google. The receptionists are very courteous. Appointments are always on time. Dr. Hwang answers all questions and explains things to you.Posted onTrustindex verifies that the original source of the review is Google. Always good service. Dr. Gupta is first rate.